Removal of a section of liver is performed for a variety of conditions, both cancerous and non-cancerous. It is a major operation and should only be performed by a surgeon experienced in liver and bile duct surgery. The liver is divided into eight separate segments and different combinations of these segments can be removed in one operation, depending on the particular condition. It a patient with a normal liver, it may be possible to remove up to 65 – 70% of the liver with excellent results. Less liver can be removed if the patient has cirrhosis. The remaining segments of liver grow larger in size to compensate for the missing piece. This growing process is usually completed within 6 weeks of surgery. It is also very common for your surgeon to remove your gallbladder at the time of liver resection whether it has gallstones or not. This is because the gallbladder is usually part of the piece of liver to be removed. Another reason for removing the gallbladder is to avoid a difficult re-operation, should you develop complications of gallstones in the future. You can live a perfectly normal life without your gallbladder.
What to expect immediately after surgery
Pain Relief
On the first day after surgery, there may be a moderate amount of discomfort at the site of the operation.
You will have some form of pain relief. There are two different options.
- epidural (if medically suitable)
- Patient controlled analgesia (PCA) and a “Painbuster” – a button you will press that causes strong pain killers to run straight into your IV line, combined with a tiny catheter in the wound providing local anaesthetic.
Your anaesthatist will discuss the pros and cons of each option with you prior to surgery. All pain relief options are not suitable for all patients.
Every effort will be made to minimize the discomfort. Your physicians and nurses will be monitoring your level of pain control frequently.
When you are back on a normal diet, you will be converted to oral pain relief.
Other Medications and Preventative Measures
You will be given Heparin twice a day as a small injection under the skin. This helps to prevent clots in the legs that may travel to the lungs and be life-threatening. In many instances you will be given a medication to decrease the acid secretions in the stomach. This prevents stomach ulcers, which also may occur after major surgery. You will be asked to wear TED stockings throughout your hospital stay. These prevent clots in the legs. You may discontinue these when you are able to get up and walk easily by yourself. A physiotherapist will see you daily whilst in the hospital. You will be shown breathing exercises and be given a breathing device (Triflow) to help to expand your lungs and prevent pneumonia.
You must not smoke at all. Post-operatively, alcohol should be avoided for at least two months if not longer, to allow your liver the best possible chance to regenerate.
Drain tubes
You will have a number of plastic tubes in your body following surgery. They will vary a little depending on your particular medical need. They will be removed at variable times following your surgery under the supervision of the surgeon.
- IV line: In your arm and in your neck (placed under anaesthesia) to give you fluids and pain relief.
- Urinary catheter: tube placed in your bladder so you don’t have to get up to pass urine.
- Abdominal drain tubes: two or three soft plastic drains coming out of your abdomen that are placed along the cut surface of your liver to drain blood or bile, so it does not collect in your abdomen.
- Stomach tube: occasionally you will wake up with a tube in your nose that goes into your stomach to stop vomiting. This will usually be removed very early after surgery.
Eating
You will not have anything to eat or drink for the one or two days after surgery. An intravenous infusion will provide you with the necessary fluids.
Your surgeon will let you know when you will be able to eat.
It is very common to lose your ability to taste food. This will return in the first month after surgery.
Urinating/Bowel Movements
During the first few days after the surgery, the tube placed in your bladder will drain your urine. You will probably not have a bowel movement until several days after the surgery.
Intensive Care
It is likely you will be looked after in intensive care for at least the first day after your surgery. Your continued stay here will depend on your condition.
Activity
You can expect your nurse and physiotherapist to help you to get out of your bed on the first day after surgery. You will be able to walk short distances even with all of the tubes and intravenous lines.
As each day passes your tolerance for walking and sitting in a chair out of bed will increase. This is extremely important to prevent pneumonia, clots in the legs and loss of general condition.
Your Incision
You can expect to have a waterproof dressing over your incision for the first five days. Your surgeon will remove the dressing at the appropriate time. You will be able to shower with the waterproof dressing on. It is quite common to have a small amount of leakage from the wound.
Most commonly, there will not be stitches to remove, they will be of the dissolving type.
Other Important Information
You can expect to see your surgeon every week day. On weekends or at times when your surgeon is operating elsewhere, you will see one of the practice partners. All are very experienced in this type of surgery and commonly assist each other in the operating theatre.
We will make every effort to keep you informed of your progress. We will always be honest and open with you and your family. Feel free to ask questions.
Length of Stay in Hospital
On average most patients will expect a 1-2 week hospital stay. This time however differs greatly for individual patients and individual operations. Some stay shorter, some much, much longer. You will not be discharged before you can walk unaided and care for yours
What are the complications that may happen immediately after surgery for liver resection?
Liver surgery is a complex procedure with many potential complications. In the hands of surgeons who are experienced, the complication rate is usually very low.
The most serious and specific complications that may be seen after this operation include:
Bleeding
Most often, this occurs during the course of your surgery. You may require a blood transfusion for this. It is uncommon to have to return to theatre post-operatively for bleeding, but certainly may occur. Approx. 15-20% of patients having liver resection will need a blood transfusion. The risks acquiring a viral disease such as Hepatitis B, C or HIV via blood transfusion are exceptionally rare.
Bile leak
When the liver is cut across, hundreds of tiny bile ducts and blood vessels have to be tied and clipped. Occasionally one of these bile ducts open-up post-operatively and leak bile. This is usually obvious in the soft drain that is left in your abdomen after the operation.
In many cases this bile leak will heal itself. If the bile leak is large in volume or becomes infected, you may require further surgery or a procedure called an ERCP. During this procedure a telescope is placed via your mouth into the bowel and a piece of plastic stent is put in the bile duct to dry up the leak. Insufficient Liver
In cases of patients with cirrhosis or patients having a large amount of liver removed, the remnant piece of liver is not enough to allow the body to function. This is often a fatal condition and is fortunately very rare. This is why all liver surgery must be carried out by an experienced surgeon. Patients with a small liver remnant after liver surgery may become jaundiced after surgery and may remain so for many months.Other immediate complications of liver surgery
Like all major surgery there are a number of serious complications that may occur. These must be dealt with on a case-by-case basis. Some of these complications are:
- Death: approx. 0.5-1% of all patients having this type of operation.
- Bleeding: either immediate or in the first 2-3 days requiring return to surgery.
- Infections: Wound, pneumonia, urine, intra-abdominal, epidural related, IV line related.
- Epidural related complications: bleeding around the spinal cord that may result in permanent paralysis. (this is extremely rare)
- A hole in the diaphragm (muscle between lungs and abdomen) that may require a tube in your chest. This is sometimes done intentionally to fully remove a tumor.
- Damage to one of the major bile ducts in the remaining liver – requiring further surgery.
- Punctured lung secondary to the IV line in your neck.
- Clots in the legs that may travel to the lungs.
- Stomach ulcer that may bleed. This may present as a vomit of blood or black bowel motions.
- Urinary catheter complications: unable to pass urine after catheter removed especially in men
- Weight loss: it is common to loose about 5-10% of starting body weight after this surgery. (approx. 5-10kg)
- Wound pain and prolonged numbness under the wound.
- Hernia of the wound.
- Bowel obstruction due to hernia or adhesions.
After discharge
What are the long-term complications after Liver Resection?
Once the recovery process is complete, there are very few long-term complications. Most complaints relate to some pain around the wound, numbness and occasionally hernias.
After any abdominal surgery there is a risk of bowel obstruction due to scar tissue forming in the abdomen.
Loss of weight
It is common for patients to lose up to 5 to 10% of their body weight compared to their weight prior to their illness. The weight loss usually stabilizes very rapidly and most patients after a small amount of initial weight loss are able to maintain their weight.
How you may feel
You may feel weak or “washed out” when you go home. You might want to nap often. Even simple tasks may exhaust you.
You might have trouble concentrating or difficulty sleeping. You might feel depressed. These feelings are usually transient and can be expected to resolve in 2-4 weeks.
Your medications
Your surgeon will discuss with you which medications you should take at home. If needed, you will go home with a prescription for pain medicine to take by mouth.
Your incision
Your dressing will be removed before you leave the hospital and if it is not leaking it will be left open to the air. You may wear loose clothing over the top of it.
Your incision may be slightly red along the cut. This is normal. If there is spreading redness or a new painful or uneven bulge appears, this is not normal and you should see your surgeon.
You may see a small amount of clear or light red fluid staining your dressing or clothes. If it is minor cover that part of the incision with a pad. If leaking is severe, or if it is pus, you should see your surgeon.
You may gently wash dried material off from around your incision. Pat your wound dry with a towel. Do not rub soap, talc or moisturizer into your incision until at least 4 weeks or until it is fully healed.
You may rub vitamin E cream onto the incision after it is fully healed.
It is normal to feel a ridge along the incision. This will go away.
It is normal to have a patch of numbness under the wound. This will not go away, but you will stop noticing it.
Over the next few months your incision will fade and become less prominent.
You deep muscle layers are sewn together with nylon stitches that do not dissolve. If you are thin, you may feel the knotted end of one of these stitches under your wound. This is harmless. If it annoys you, it can be easily removed at some time after your surgery. Occasionally a stitch may poke out of your wound. This is quite safe. See your surgeon in an elective manner if this occurs.
Activity
Do not drive until you have stopped taking narcotic pain medication and feel you could respond in an emergency.
You may climb stairs.
You may go outside, but avoid traveling long distances until you see your surgeon at your next visit.
Don’t lift more that 10 kg for 6 weeks. (This is about the weight of a briefcase or a bag of groceries) this applies to lifting children, but they may sit on your lap.
You may start some light exercise when you feel comfortable.
You may swim after 4 weeks
Heavy exercise may be started after 6 weeks – but use common sense and go slowly at first.
You may resume sexual activity when you feel ready unless your doctor has told you otherwise. Costs to be incurred from this surgery
The surgeons in this practice do not charge any out of pocket expenses for your in hospital stay. We will bill your health fund directly.
The health funds do not cover outpatient care and there will be some out of pocket fees for the initial outpatient consultations.
There may be other out-of-pocket fees from your anaesthetist and any other specialists who are asked to look after you. You should ask them ahead of time any out of pocket costs. Ask your surgeon who will be performing your anaesthetic and you can make enquiries with them about any out-of-pocket expenses.
The operation
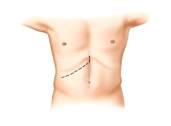
The operation for removing a section of liver varies depending on what segments are to be removed. More common operations are to remove the whole right side, or whole left side. This will be discussed at length with you by your surgeon. The operation is carried out by tying and stapling hundreds and hundreds of bile ducts and blood vessels in the liver and dividing the liver with a clean cut. The incision will be in the upper part of your abdomen and either look like a hockey stick or occasionally like a Mercedes Benz sign.
